Estrogen Patch Shortage: FDA’s Warning Removal Fuels Demand Surge
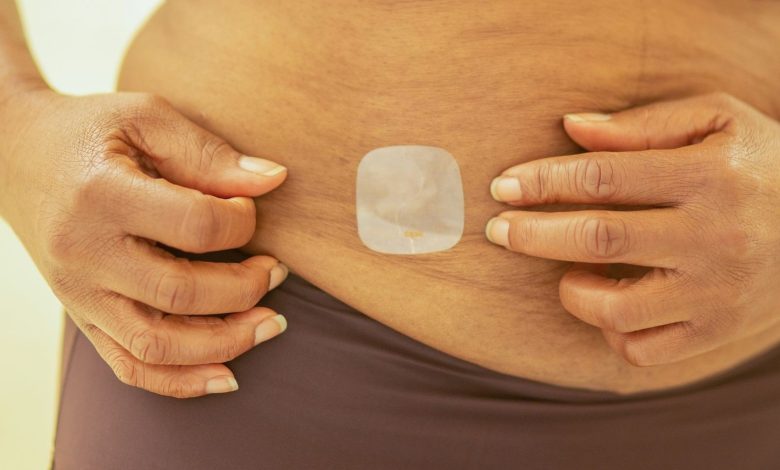
Introduction
Estrogen, a primary female sex hormone, plays a crucial role in numerous bodily functions, including the regulation of the menstrual cycle, bone density, and cardiovascular health. Hormone Replacement Therapy (HRT), particularly the estrogen patch, has become a common treatment for managing menopausal symptoms such as hot flashes, night sweats, and vaginal dryness. However, recent events have brought this therapy into the spotlight due to a significant surge in demand coupled with supply challenges. The Food and Drug Administration’s (FDA) decision to remove the black box warning from hormone replacement therapies late last year has inadvertently fueled a boom in the therapy’s popularity, leading to shortages of the most insured type—the estrogen patch. This article delves into the complexities of this situation, exploring the factors contributing to the shortage, the impact on patients and healthcare providers, and potential solutions to mitigate the crisis.
Background on Hormone Replacement Therapy
Hormone Replacement Therapy (HRT) has a long and somewhat controversial history. Initially, it was widely prescribed to women experiencing menopause to alleviate symptoms and prevent long-term health issues such as osteoporosis and heart disease. The treatment typically involves supplementing declining hormone levels, primarily estrogen and sometimes progesterone, to restore hormonal balance. The estrogen patch, a transdermal delivery system, has become a popular choice due to its ease of use and consistent hormone release, which can minimize side effects compared to oral medications.
In the early 2000s, a large study by the Women’s Health Initiative (WHI) raised concerns about the safety of HRT, particularly the combination of estrogen and progestin. The study linked HRT to an increased risk of breast cancer, heart disease, and stroke, leading to a significant decline in its use. Consequently, the FDA added a black box warning to HRT products, highlighting these potential risks. However, subsequent research and re-evaluations of the WHI data have provided a more nuanced understanding of HRT, suggesting that the risks may vary depending on the type of hormone, dosage, and individual health factors, particularly the age at which HRT is initiated. For instance, initiating HRT closer to the onset of menopause is now considered to have a more favorable risk-benefit profile for many women.
FDA’s Decision to Remove the Black Box Warning
In November of the previous year, the FDA made a significant decision to remove the black box warning from certain hormone replacement therapies. This decision was based on evolving scientific evidence that provided a more refined understanding of the risks and benefits associated with HRT. The FDA recognized that the blanket warning was overly broad and did not accurately reflect the varied risk profiles of different HRT regimens. By removing the warning, the FDA aimed to provide healthcare providers and patients with more accurate and balanced information to make informed decisions about HRT use.
FDA chief Dr. Marty Makary noted that the agency’s move was intended to reflect the latest scientific evidence and encourage more open discussions between doctors and patients about the potential benefits and risks of HRT. The removal of the black box warning was expected to lead to a more individualized approach to HRT, where treatment decisions are tailored to the specific needs and health status of each patient. However, the agency did not anticipate the tremendous surge in demand for estrogen patches that would follow, creating unforeseen supply challenges.
The Unprecedented Surge in Demand
Following the FDA’s decision, there was an immediate and substantial increase in the demand for estrogen patches. Dr. Robert Kauffman, a professor of obstetrics and gynecology at Texas Tech Physicians of Amarillo, noted, “There’s been a surge in demand for the last two or three years where the utilization of transdermal estrogen has gone up significantly.” This surge can be attributed to several factors. First, the removal of the black box warning likely alleviated some of the fears and concerns that had previously deterred women from considering HRT. Second, increased awareness and education about the benefits of HRT, particularly in managing menopausal symptoms and improving quality of life, have also contributed to the rising demand. Third, the aging population and the growing number of women entering menopause have naturally increased the overall demand for HRT.
The estrogen patch, in particular, has seen a significant increase in popularity due to its convenience, ease of use, and perceived lower risk profile compared to oral estrogen. Transdermal estrogen bypasses the liver, reducing the risk of certain side effects associated with oral administration. This has made it a preferred choice for many women and healthcare providers. However, the sudden and rapid increase in demand has placed significant strain on the supply chain, leading to shortages and difficulties in obtaining certain doses of estrogen patches.
Supply Chain Challenges and Shortages
Despite the increased demand, the FDA has not yet included estrogen patches on its list of drugs in shortage. However, doctors and patients across the country report difficulties in obtaining specific dosages of estrogen patches. This discrepancy may be due to the FDA’s criteria for declaring a drug shortage, which typically involves a complete inability to meet demand across the board. In the case of estrogen patches, some manufacturers may still be able to supply certain dosages, while others are experiencing significant backorders and delays.
Several factors may be contributing to the supply challenges. Manufacturing capacity, raw material availability, and regulatory hurdles can all play a role in limiting the production and distribution of estrogen patches. Additionally, the pharmaceutical industry has faced broader supply chain disruptions in recent years due to global events such as the COVID-19 pandemic, which have further exacerbated the problem. These disruptions can affect the availability of raw materials, packaging components, and transportation services, all of which are essential for the production and distribution of medications.
The intricacies of pharmaceutical manufacturing also contribute to potential bottlenecks. Producing hormone patches requires precise processes to ensure accurate dosing and consistent hormone release. Any deviations or delays in these processes can impact the overall supply. Furthermore, stringent quality control measures and regulatory inspections can add to the time and cost of production.
Expert Opinions on the Shortage
Experts in the field of obstetrics and gynecology have expressed concerns about the estrogen patch shortage and its potential impact on patient care. Dr. Robert Kauffman has highlighted the significant increase in demand and the challenges healthcare providers face in securing adequate supplies for their patients. Other experts have echoed these concerns, emphasizing the need for better communication and coordination between manufacturers, distributors, and healthcare providers to address the shortage effectively.
Some experts have suggested that the FDA should consider implementing measures to alleviate the supply challenges, such as expediting the approval of new manufacturers or increasing production quotas for existing manufacturers. Others have called for greater transparency in the supply chain, allowing healthcare providers to better anticipate and manage potential shortages. Additionally, some experts have advocated for increased education and awareness about alternative HRT options, such as compounded hormones or other delivery methods, to help patients navigate the shortage.
Impact on Patients and Healthcare Providers
The estrogen patch shortage has had a significant impact on both patients and healthcare providers. For patients, the shortage can lead to interruptions in their treatment, causing a resurgence of menopausal symptoms and a decline in their quality of life. The uncertainty and anxiety associated with not being able to obtain their medication can also be distressing.
Healthcare providers face the challenge of managing patients who are unable to obtain their usual estrogen patch dosage. This may involve switching patients to alternative HRT regimens, adjusting dosages, or exploring other non-hormonal treatments for menopausal symptoms. These changes can be time-consuming and may require additional patient education and monitoring. Moreover, the shortage can strain the relationship between patients and providers, as patients may feel frustrated or abandoned by the healthcare system.
Furthermore, the shortage can disproportionately affect certain populations, such as women with limited financial resources or those living in rural areas with limited access to healthcare. These women may face additional barriers in obtaining alternative treatments or navigating the healthcare system to find solutions.
Alternative HRT Therapies and Considerations
Given the challenges associated with the estrogen patch shortage, it is essential for patients and healthcare providers to consider alternative HRT therapies and management strategies. Several options are available, each with its own advantages and disadvantages. Oral estrogen, for example, is a widely available alternative, although it may carry a slightly different risk profile compared to transdermal estrogen. Topical estrogen creams and gels can also be used to treat vaginal dryness and other localized symptoms.
Compounded hormones, which are custom-made by a pharmacist, offer another alternative. Compounding allows for individualized hormone formulations and dosages, which may be beneficial for patients who have specific needs or sensitivities. However, compounded hormones are not FDA-approved and may not be subject to the same quality control standards as commercially available medications.
Non-hormonal treatments for menopausal symptoms include lifestyle modifications such as regular exercise, a healthy diet, and stress reduction techniques. Certain medications, such as selective serotonin reuptake inhibitors (SSRIs) and gabapentin, can also help manage hot flashes and other symptoms. Additionally, alternative therapies such as acupuncture and herbal remedies may provide relief for some women.
The choice of HRT therapy should be individualized based on the patient’s specific symptoms, medical history, and preferences. Healthcare providers should carefully weigh the risks and benefits of each option and provide patients with comprehensive information to make informed decisions.
FDA’s Response and Monitoring
While the FDA has not yet declared an official shortage of estrogen patches, the agency is closely monitoring the situation and working with manufacturers to address the supply challenges. The FDA’s role in managing drug shortages involves assessing the availability of medications, identifying potential causes of shortages, and working with manufacturers to increase production or find alternative sources of supply.
The FDA also collaborates with other government agencies, healthcare providers, and patient advocacy groups to ensure that patients have access to the medications they need. In some cases, the FDA may expedite the approval of new manufacturers or allow for the importation of medications from other countries to alleviate shortages.
Given the evolving nature of the estrogen patch supply situation, it is essential for healthcare providers and patients to stay informed about the latest developments and recommendations from the FDA. The agency’s website provides up-to-date information on drug shortages and other relevant topics.
Global Perspective on HRT Supply
The shortage of estrogen patches is not unique to the United States. Other countries around the world have also experienced similar challenges in recent years. Factors such as global supply chain disruptions, manufacturing capacity limitations, and regulatory hurdles can all contribute to these shortages.
In some countries, governments have implemented measures to mitigate drug shortages, such as stockpiling essential medications, diversifying sources of supply, and incentivizing domestic production. International collaboration and information sharing can also help address global drug shortages more effectively.
Market Analysis and Future Projections
The global market for hormone replacement therapy is expected to continue to grow in the coming years, driven by the aging population, increasing awareness of the benefits of HRT, and the development of new and improved therapies. However, supply chain challenges and regulatory uncertainties could impact the growth trajectory of the market.
Market research firms project that the demand for transdermal estrogen, including patches, will continue to rise, driven by its convenience and perceived safety advantages. Manufacturers are investing in expanding their production capacity to meet this growing demand. However, it remains to be seen whether these efforts will be sufficient to prevent future shortages.
A comparison table of different HRT options is shown below:
| HRT Option | Pros | Cons | Considerations |
|---|---|---|---|
| Estrogen Patch | Convenient, consistent hormone release, bypasses liver | Potential for skin irritation, possible shortage | Monitor skin reaction, check availability |
| Oral Estrogen | Widely available, easy to administer | May increase risk of blood clots, impacts liver | Monitor liver function, consider risk factors |
| Topical Estrogen | Localized treatment, minimal systemic absorption | May not be effective for all symptoms, application requirements | Use for vaginal dryness, follow application instructions |
| Compounded Hormones | Customized formulations, tailored dosages | Not FDA-approved, variable quality control | Discuss with a knowledgeable pharmacist |
| Non-Hormonal Treatments | Avoids hormone-related risks, can improve overall health | May not be as effective for all symptoms, requires lifestyle changes | Combine with healthy habits, consider medications |
Conclusion
The estrogen patch shortage is a complex issue with multiple contributing factors, including the FDA’s decision to remove the black box warning, increased demand for HRT, and supply chain challenges. While the FDA continues to monitor the situation and work with manufacturers to address the shortage, it is essential for healthcare providers and patients to explore alternative HRT therapies and management strategies. By staying informed, communicating effectively, and making individualized treatment decisions, women can continue to manage their menopausal symptoms and improve their quality of life. The situation also highlights the need for a more resilient and transparent pharmaceutical supply chain to prevent future shortages and ensure that patients have access to the medications they need.
Furthermore, the events surrounding the estrogen patch shortage underscore the importance of evidence-based decision-making in healthcare. While the FDA’s decision to remove the black box warning was based on evolving scientific evidence, the agency did not fully anticipate the potential consequences of this decision on the supply chain. This highlights the need for ongoing monitoring and evaluation of healthcare policies to ensure that they are both evidence-based and practical.
In the long term, addressing the estrogen patch shortage will require a multi-faceted approach involving manufacturers, distributors, healthcare providers, policymakers, and patients. By working together, these stakeholders can help ensure that women have access to safe and effective HRT options and that the pharmaceutical supply chain is resilient enough to meet the growing demand for these medications. For instance, promoting the research and development of novel HRT delivery systems can help diversify the market and reduce reliance on a single type of product, such as the estrogen patch. Additionally, fostering greater transparency and collaboration among manufacturers and distributors can help improve supply chain efficiency and prevent future shortages.
The interplay between policy decisions, market dynamics, and patient needs is evident in this scenario. As the population ages and awareness of HRT benefits grows, the demand for such treatments will likely increase. Therefore, proactive planning and strategic initiatives are essential to ensure a stable and reliable supply of these critical medications.
Moreover, it is crucial to address the underlying factors that contribute to drug shortages, such as manufacturing capacity limitations, regulatory hurdles, and supply chain vulnerabilities. This may involve investing in domestic manufacturing capacity, streamlining regulatory processes, and diversifying sources of supply. By taking these steps, we can create a more resilient and sustainable pharmaceutical supply chain that is better equipped to meet the needs of patients in the years to come.
This situation also underscores the importance of ongoing education and awareness about HRT and its potential benefits and risks. By providing healthcare providers and patients with accurate and balanced information, we can empower them to make informed decisions about their health and well-being. Additionally, promoting open and honest communication between patients and providers can help build trust and facilitate shared decision-making.
In conclusion, the estrogen patch shortage is a complex and multifaceted issue that requires a comprehensive and collaborative approach. By addressing the underlying causes of the shortage, investing in a more resilient pharmaceutical supply chain, and promoting education and awareness, we can help ensure that women have access to the safe and effective HRT options they need to manage their menopausal symptoms and improve their quality of life. Additionally, keeping track of events such as the killing of Casey Goodson Jr are important to staying informed about current affairs.
The developments around HRT supply also have implications for broader healthcare policy and pharmaceutical regulations. As evidenced by the unconstitutional grants halted by the Trump administration, regulatory decisions can have wide-ranging effects.
This also is relevant to WHO data access .



